Much of the research on whiplash injuries over the last few years has focused on the ligaments of the spine as the source of chronic pain and loss of function. Ligament injuries are problematic for two reasons: first, such injuries can be impossible to detect using plain x-rays or CT scans; and, second, torn ligaments can cause permanent disability if untreated.
A 2004 study1 found that the transverse ligament could be injured from rear-end collisions. A new study2 from Norway adds some exciting new insight to the nature of ligament injuries from auto collisions, and provides some new information on the role of head position at the time of the collision.
Previous researchers have found that head position can be an important risk factor in whiplash; patients who have their heads turned at the moment of the crash are much more likely to be injured. This is due to the fact that combined extension of the neck with rotation places severe strains on the ligaments of the spine.
To investigate this issue, the authors of this recent study2 performed MRIs on 92 whiplash patients and 30 healthy control subjects. All of the whiplash patients had normal x-ray results one week after the collision. The MRI was performed an average of six years after the collision.
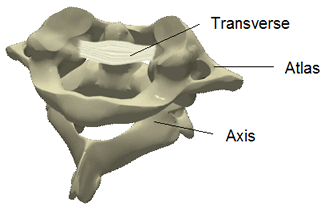
The transverse ligament limits the motion of the
1st Cervical Vertebrae (Atlas) and the 2nd Cervical
Vertebrae (Axis). If the head is turned during a
rear-end collision, this ligament can be stretched
or torn, resulting in chronic pain and loss of neck function.
The authors found significant differences between the whiplash patients and control subjects:
- “For all the neck structures considered, the chronic whiplash patients had significantly more MRI high-grade changes than the controls…”
- The alar ligament was the most commonly injured structure, as 66% of the whiplash patients showed significant damage to the ligament.
- “The patients who had the head rotated at the instant of collision had more often high-grade MRI changes of the alar ligaments than those with the head in a neutral position. A total of 61.7% of the patients with rotated neck position had alar ligament grade 3 lesions, as opposed to only 4.4% in the patient group with neutral neck position.”
- “The association between head position and high-grade lesions (grade 2-3) of the alar ligaments was more pronounced in rear-end…than in front collisions.”
- “High-grade lesions to the transverse ligament were also more common among patients with the head turned at the instant of the collision. Similar results appeared for the tectorial membrane, although with rather few high-grade changes.”
- “Severe MRI changes in the transverse ligament and the posterior atlanto-occipital membrane were considerably more common in front-end than in rear-end collisions.”
This study provides some very important findings relevant for those who represent whiplash injury patients:
- Front-end collision can cause ligament injury from hyper-flexion. The authors write that, “front-end collisions should be included in the definition of potential causes of a whiplash trauma, not only rear-end or side impact.”
- Head position is an important risk factor in whiplash injuries, as a turned head at the time of impact dramatically increases the changes of ligament injury. When working with whiplash patients, it is critical to take a careful history, with particular emphasis on the position of the occupant’s head at the time of impact.
- MRI exams of the ligaments of the upper cervical spine can be a useful tool in diagnosing chronic whiplash pain. The authors of this study looked for increased signal intensity in the affected structures.
The authors conclude their study, “the difference in MRI-verified lesions between [whiplash] patients and control persons, and in particular the association with head position and impact direction at the time of the accident, indicate that these lesions are caused by the whiplash trauma.”
- Krakenes J, Kaale BR, Nordli H, Moen G, Rorvik J, Gilhus NE. MR analysis of the transverse ligament in the late stage of whiplash injury. Acta Radiologica 2003;44:637-644.
- Kaale BR, Krakenes J, Albrektsen G, Wester K. Head position and impact direction in whiplash injuries: associations with MRI-verified lesions of ligaments and membranes in the upper cervical spine. Journal of Neurotrauma 2005;22(11):1294-1302.